How to protect yourself from sudden death
Insights from a cardiologist on why healthy people can still be at risk and what screening can reveal

You probably know someone who has passed away “suddenly.” No long illness, no clear warning, just a shocking phone call or message that leaves everyone asking the same question, “How could this happen?”
Most people rely on routine health check-ups to reassure themselves that everything is fine. Blood tests are normal, blood pressure is stable, and the ECG shows no obvious problems. It appears like a clean bill of health. But sudden death can still occur in people who appear perfectly healthy. The Thaiger talked to Dr Sureerat Panyarachun of MedPark Hospital to understand why this can happen even when test results appear normal, and what can be done to reduce the risk.
What is sudden death?
In medical terms, sudden death refers to an unexpected natural death that happens within minutes or within one hour after symptoms begin. It doesn’t only mean a heart attack, as it may include deaths caused by abnormal heart rhythms, inherited heart muscle diseases, epilepsy-related events, and certain types of stroke. It usually happens quickly, where the body shuts down before help can arrive.
Dr. Sureerat explains that heart rhythm problems are a big part of it. The heart depends on electrical signals to pump blood properly. If those signals suddenly become chaotic, the heart can stop pumping effectively. This can happen even when the arteries are not blocked. That is why a person with normal cholesterol and blood pressure can still be at risk.
In addition to the heart, the brain can also be the culprit. Some medical conditions, such as epilepsy-related complications, major strokes, and bleeding in the brain, can cause death to occur suddenly without warning. Because sudden death can come from different organs, it cannot be prevented with one simple test. A broader view of risk is needed.
Can sudden death occur in younger people?
Many people assume it is something that happens only to older adults or those with serious diseases. In reality, younger people with no symptoms can also be affected.
Doctors divide sudden death risk by age because the causes differ. In younger people, inherited heart muscle disease and electrical disorders are more common. These affect how the heart contracts or how its rhythm is controlled. This explains why athletes sometimes collapse suddenly despite being fit and active. In older adults, sudden death is more often linked to coronary artery disease or stroke. Blocked arteries can trigger fatal heart rhythms, while weakened blood vessels in the brain can rupture or clot.
Dr. Sureerat notes that the modern lifestyle has blurred this line. Stress, obesity, diabetes, and sleep problems are now affecting people at younger ages. This is important because younger people are less likely to suspect danger. They exercise, work long hours, and feel healthy. But genetic conditions and lifestyle risks can combine quietly. Without targeted screening, problems can remain hidden until the first symptom, collapse, occurs.
Why do routine check-ups miss hidden dangers?
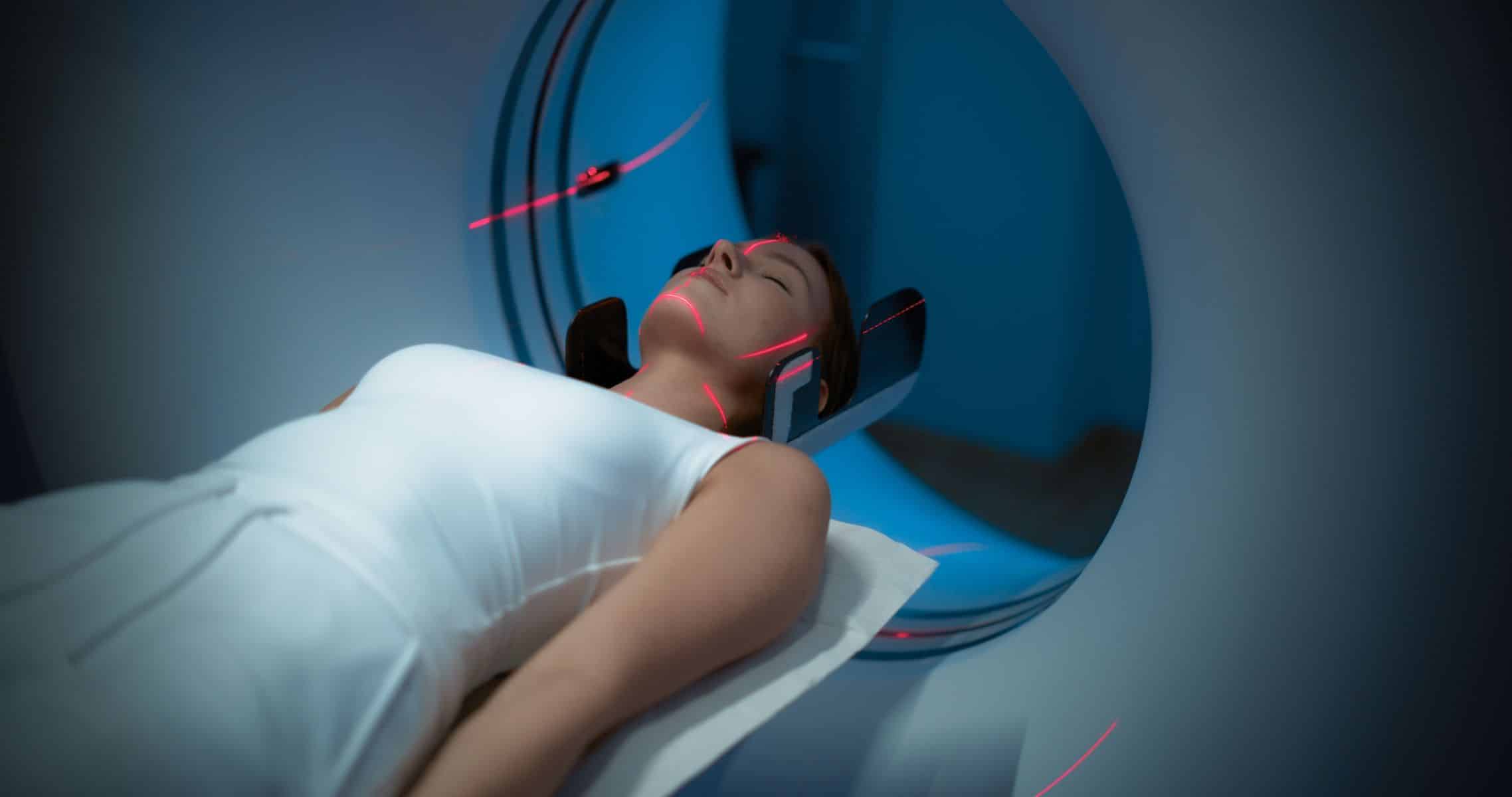
Routine check-ups are designed to detect common conditions like diabetes, high cholesterol, and high blood pressure. They are not designed to find rare electrical heart disorders, early structural heart disease, or brain-related causes of collapse. Dr. Sureerat explains that important areas are usually not tested, such as the whole aorta, the brain’s blood vessels, and extended-interval rhythm monitoring.
Some dangerous rhythm problems appear only once every few days. A short ECG taken in a clinic can easily miss them. Genetic conditions also remain invisible unless tested directly. Even sleep disorders are often ignored unless someone complains strongly about symptoms.
This creates a false sense of safety. A person may be told their heart is normal while carrying a rhythm disorder that appears only at night or during stress. The absence of symptoms does not mean the absence of disease. It only means the disease has not yet revealed itself.
What are some early clues people ignore?
Sudden death is often described as silent, but small warning signs can appear. Chest tightness, breathlessness, dizziness, palpitations, or fainting may be dismissed as stress or exhaustion. Dr. Sureerat also points out that heart-related pain can feel like indigestion rather than sharp chest pain.
Neurological signs may also be overlooked. Headaches, blurred vision, or brief blackouts may suggest brain involvement rather than heart disease. Silent seizures can cause a short loss of consciousness without obvious convulsions. People often fail to link these symptoms to serious risk because they come and go.
Your lifestyle can also be an early clue. Smoking, alcohol use, and stimulant drugs increase vulnerability. Emotional stress and physical strain also raise the chance of rhythm problems. Sudden death is rarely due to a single factor. It usually stems from several risks building up unnoticed.
Who faces the highest risk today?
Dr. Sureerat Panyarachun explains that the risk of sudden death is not evenly spread across the population. While it can occur in anyone, certain groups face a much greater danger because of underlying heart, brain, or genetic conditions, as well as lifestyle and environmental pressures that affect how the body’s vital systems function under stress. She identifies the following high-risk groups:
- Young athletes with undiagnosed inherited heart muscle disease
- Adults who have previously suffered a heart attack
- People with genetic heart rhythm syndromes, such as Long QT syndrome or Brugada syndrome, where the heart’s electrical system can become ineffectual without warning
- Patients with epilepsy are at risk of sudden neurological shutdown
- People with sleep apnoea, obesity, or diabetes, which place long-term strain on both the heart and the brain
- Those with a family history of unexplained sudden death, as genetic links can run through generations
- Individuals who misuse substances such as cocaine, which can trigger fatal heart rhythm disturbances
- People living under prolonged emotional stress, since stress hormones can interfere with the heart’s electrical stability.
Can advanced screening prevent sudden death?
Advanced screening looks beyond routine tests. It includes heart imaging, extended-interval rhythm monitoring, brain scans, genetic testing, and sleep studies. These tools uncover problems that would otherwise remain hidden.
Dr. Sureerat recalls a 28-year-old man who appeared fit but had a family history of sudden death. “His ECG showed a slightly long QT,” she says. Genetic testing confirmed the disorder. He had no symptoms. His electrophysiology study showed low risk. In other cases such as Brugada syndrome, after typical screening EKG, family history of sudden death, genetic testing, and high-risk electrophysiology study results, he proceeded to have ICD with regular follow up. Treatment and monitoring were started early.“ This exemplifies why specific screening is important,” she says.
In another case, an aortic aneurysm was found before rupture. Careful monitoring and later intervention prevented a fatal outcome. These cases show how early detection transforms sudden death from a random event into a manageable risk.
What happens after risk is found
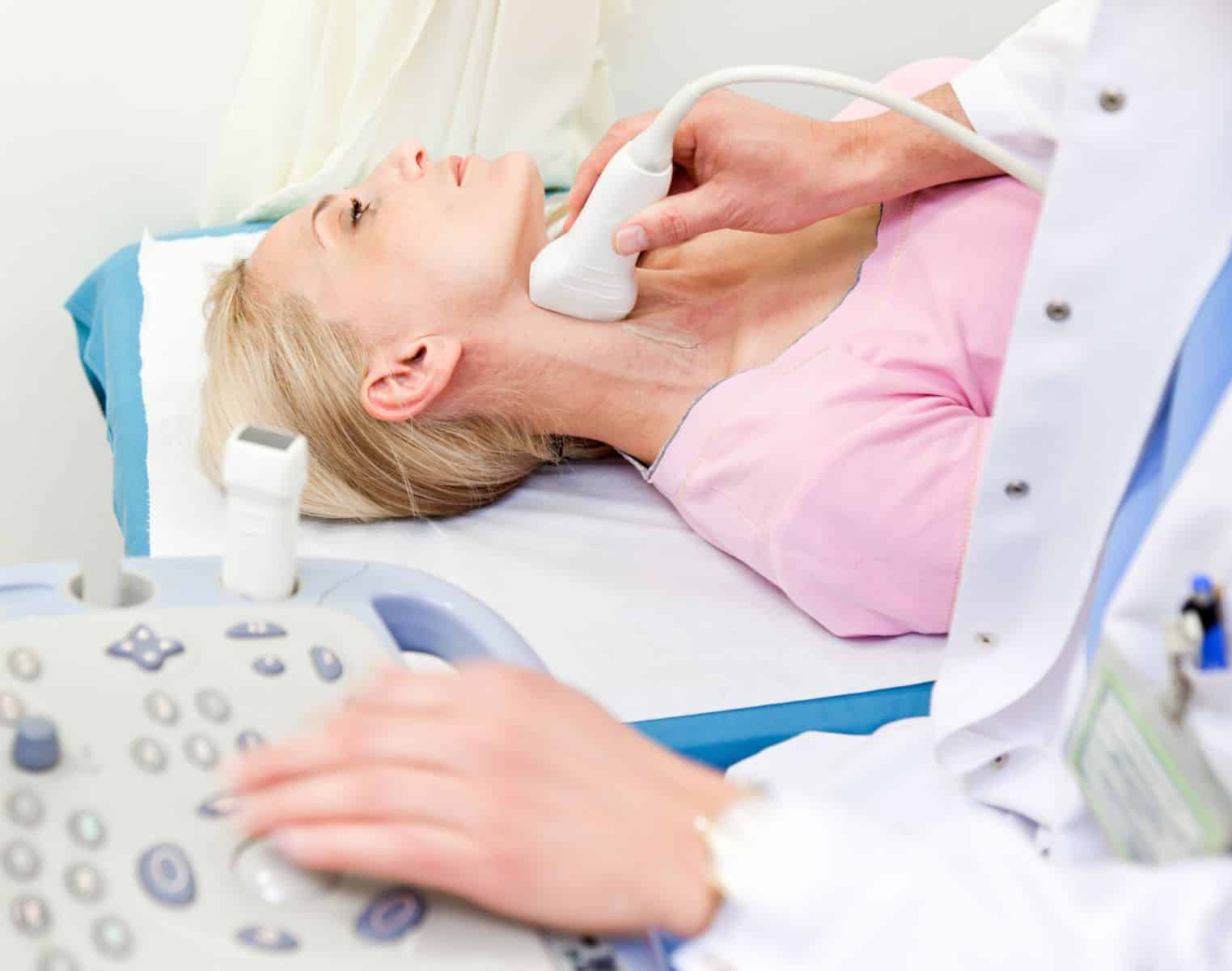
Finding risk is only the beginning. Dr. Sureerat explains that patients enter a structured, long-term follow-up program. They receive regular heart rhythm tests and heart scans. Genetic counselling is repeated when needed. Devices such as pacemakers or implantable defibrillators are checked carefully.
Sleep studies are added when breathing problems are suspected. Neurologists may join the care team for epilepsy-related risk. Family members may also be screened because inherited conditions often affect close relatives.
Education is part of prevention. Patients learn emergency response skills and may be advised to keep defibrillators at home or work if the risk is high. Prevention becomes a system, not a single appointment.
The right screening can reduce your risk.
“Sudden death is often silent,” Dr. Sureerat says, “but it doesn’t have to be. One specific check-up could save a lifetime.” Feeling healthy is not the same as being risk-free. If there is a family history, fainting, seizures, heavy snoring, or persistent stress alongside other risk factors, more extensive screening may be worth considering.
Sudden death cannot always be prevented, but many cases can be delayed or avoided. The difference lies in whether the hidden danger is looked for before it has a chance to strike. Visit MedPark Hospital for a sudden death screening and uncover whether hidden risks are present. Its focused screening programme looks specifically for heart rhythm disorders, neurological conditions, and inherited factors that routine check-ups often miss, helping turn uncertainty into clear medical guidance.
Sponsored
Latest Thailand News
Follow The Thaiger on Google News:


























